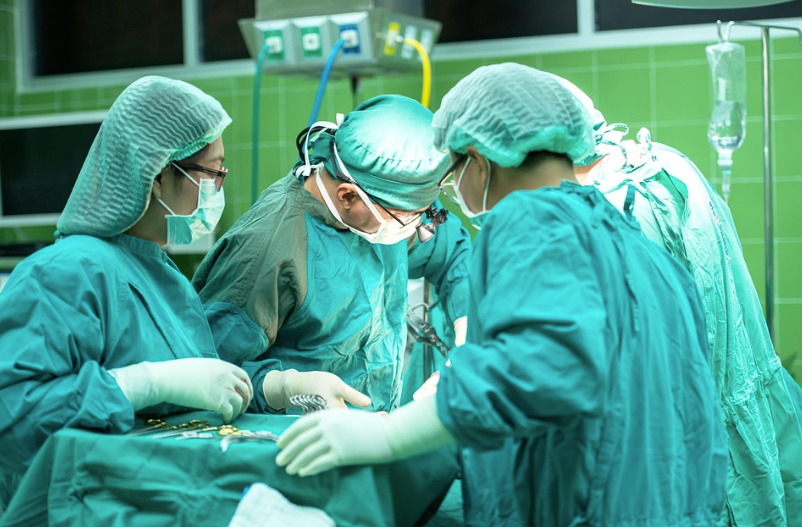
 Hysterectomy is one of the most frequently performed surgeries for women in gynecology. With recent advances in medicine, the procedure has become relatively simple and quick. Whether it is a subtotal hysterectomy removing only the uterine body or a total hysterectomy, specialists can perform the operation efficiently.
Hysterectomy is one of the most frequently performed surgeries for women in gynecology. With recent advances in medicine, the procedure has become relatively simple and quick. Whether it is a subtotal hysterectomy removing only the uterine body or a total hysterectomy, specialists can perform the operation efficiently.
Professor Lin Zhongqiu, Director of Gynecologic Oncology at Sun Yat‑sen Memorial Hospital, notes that while national statistics on hysterectomy rates in China are unavailable, he personally performs seven to eight such operations each week — a clear indicator of how many women lose their uterus.
The Alarming Number of Hysterectomies
There are two main scenarios for hysterectomy in hospitals. The first is for pathological uterine conditions requiring surgical treatment. The second involves women who have already given birth requesting hysterectomy because they view menstruation as inconvenient or suffer from painful periods. This is partly encouraged by some medical providers, such as the claim that the uterus is unnecessary after childbirth, and may also serve as a way to increase medical income. Similar patterns and high hysterectomy rates have been reported in Taiwan.
Uterine fibroids, the most common benign tumor of the female reproductive system, affect 20% to 25% of women aged 30 to 50. Nearly one in four women over 35 develops fibroids, and their incidence has been increasing in recent years. Since the malignant transformation rate of fibroids is only about 1%, hysterectomy is usually unnecessary unless fibroids cause heavy menstrual bleeding, dysmenorrhea, infertility, or recurrent miscarriage. Yet due to conventional clinical thinking, prophylactic hysterectomy is often recommended as a permanent solution to prevent potential malignant change.
Four Reasons Against Unnecessary Hysterectomy
In reality, many women undergo hysterectomy unnecessarily. Despite having performed thousands of hysterectomies, Professor Lin Zhongqiu does not advocate removing the uterus without careful consideration, for the following four reasons:
- There are three main surgical approaches: open abdominal hysterectomy, transvaginal hysterectomy, and laparoscopic hysterectomy. Any surgery, regardless of scale, is invasive and affects physical health to some degree.
- No surgery is free from the risk of complications. Even simple procedures may lead to issues such as intestinal adhesions, and pelvic surgery carries a risk of injury to the bladder, intestines, and other adjacent organs.
- Surgical accidents may occur, including risks related to anesthesia.
- Even if the surgery is completely successful with no complications, hysterectomy can impair ovarian function. The uterus and ovaries share an interconnected blood supply; when the uterus is removed, approximately 30% of ovarian blood flow — supplied by branches of the uterine artery — is lost. Reduced blood perfusion compromises ovarian function, which may lead to premature menopause, menopausal symptoms, and even accelerated aging.